The Many Faces of Iliacus Dysfunction
by Stephen O’Dwyer, CNMT
Iliacus Dysfunction comes in many shapes and sizes. If you're experiencing chronic or recurrent pain (or tingling, numbness, aching, or hot/cold sensations) in any of the following regions...
Lower abdomen
Groin
Buttocks
Down the leg
Hip Joint
Lower back
Sacroiliac Joint
Across the top of the hip bone (iliac crest)
Wrapping around to the lower back or buttocks
... and these symptoms have not responded to treatments such as injections, physical therapy, rest, etc. and/or the diagnosis has been inconclusive or vague, then you may be suffering from Iliacus Dysfunction, a symptom of Iliopsoas Syndrome.
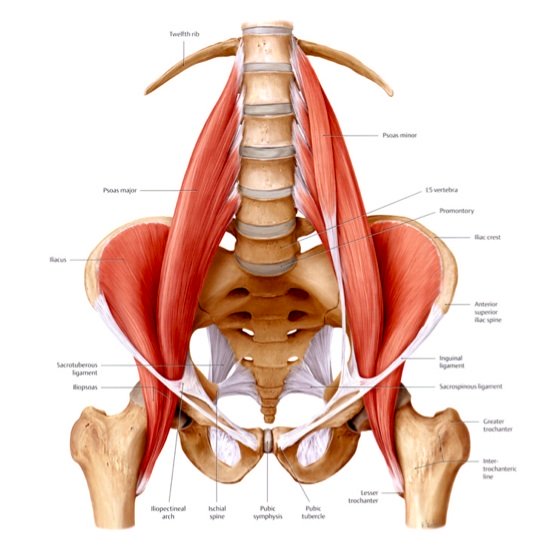
Anatomy of the Iliacus and Psoas (collectively called the Iliopsoas)
Tucked inside your hip bone and hidden from easy hands-on access lies one of the most potentially troublesome muscles in the body: the iliacus muscle.
This muscle is the often-ignored neighbor of the more well-known psoas muscle.
Together the iliacus and psoas are often referred to collectively as the iliopsoas because they share a common attachment at the upper inner thigh, the lesser trochanter.
Here's what the two muscles look like together:
The muscle attaching along the lumbar spine is the psoas.
While they are both primary hip flexors with a common attachment, they are distinct muscles and can cause unique problems.
Here I will focus on the iliacus. Over many years of treating chronic pain I have found that this muscle is the root of much unexplained misery.
What's the Basic Problem?
One very common problem of the iliacus is that it can shorten over time. This can be due to prolonged sitting and/or driving and the absence of regular stretching. Shortness in this muscle can be a particularly tenacious problem in athletes who don't stretch enough because their iliacus muscles may be quite strong.
A strong, flexible, resilient muscle is a good thing.
But a strong, dense, short, inflexible muscle is not.
Prolonged sitting with the iliacus in a shortened state, or just the lack of stretching over time, can lead to the iliacus adapting to a shortened length. Once a muscle becomes adapted to a particular length, this is its natural state or typical state.
Once in an adapted state, the iliacus has trouble returning to its normal resting length. And this is where the trouble starts.
Chronic Muscular Contraction
If a muscle cannot return to its normal, healthy resting length, it then resides in a state of chronic contraction and numerous undesirable consequences can result:
A chronically contracted iliacus can become ischemic (low blood flow). Imagine the white knuckles of a clenched fist. No blood flow there. An ischemic muscle is often a painful muscle.
A chronically contracted iliacus can develop trigger points which refer pain (or numerous other possible sensations – thermal, tingling, numbness, aching) either radiating out from the muscle or felt in other parts of the body. Triggers points in the iliacus can refer sensation to the groin, the hip, down the leg, etc.
A chronically contracted iliacus can distort the movement of the hip joint. For example, movement at the front of the hip joint could be reduced or restricted thus overworking other muscles in the hip.
A chronically contracted iliacus can cause a variety of compensations or distortions in the body. If, for example, a tight iliacus reduces movement in one hip, then the other hip or the spine or other parts of the body may be called upon to compensate and change their normal pattern of movement.
A chronically contracted iliacus can promote pelvic torsion (aka a twisted pelvis) which results in a functional leg-length difference and disruption of the body’s neutral relationship with gravity.
Potential Regions of Pain Due to Iliacus Dysfunction
What this means for an individual whose iliacus is tight and short and ischemic (low blood flow) is that pain might be experienced in any of a variety of places in the body. During my years of treating iliacus dysfunction, clients have presented with pain in all following areas of the body:
Lower abdomen
Groin
Buttocks
Down the leg
Hip Joint
Lower back
Sacroiliac Joint
Across the top of the hip bone (iliac crest)
Wrapping around to the lower back or buttocks
The problem an individual may face when being examined by a physician not trained in soft tissue problems is that examination of any of the above areas of pain may reveal exactly nothing.
Many standardized allopathic tests, including neurologic tests, will come back negative because they are not designed to evaluate soft tissue problems. Such problems can only be properly assessed by seeing the whole body as an integrated system.
When no obvious trauma exists, looking for defects in individual body parts is much like standing too close to a painting: you can’t actually see the painting when you’re, say, one inch away from it. You might see brush strokes, but you can’t see the whole painting. You need to step back in order to see the whole and have perspective.
Of particular difficulty in the case of the iliacus is the fact of its hidden location. This muscle is not easy to palpate without proper guidance.
can the iliacus be stretched out?
It can be stretched out, yes, but when a muscle has adapted into a fixed pattern it can easily return to its tight, adapted state. This is why we can feel caught in a cycle of constant stretching that doesn't seem to last.
Additionally, many of us still utilize a static stretching method which can trigger the Protective Stretch Reflex. If you’ve ever held a muscle on a static stretch for 30-60 seconds or longer but felt your body trembling and the muscle fighting you, then you’ve experienced this protective reflex.
The Protective Stretch Reflex exists to prevent serious injury but unfortunately can be triggered in as little as 5 seconds of holding a stretch.
This is why I strongly recommend using Active Isolated Stretching instead. With this stretching method, we use a repeated 2-second stretch instead.
pelvic torsion & ILIACUS DYSFUNCTION
Lastly, it’s important to consider the relationship between iliacus dysfunction and pelvic torsion.
Pelvic torsion is a widespread but poorly understood problem can be responsible for a wide range of bewildering symptoms and persistent pain that don’t seem to respond to treatment.
The immediate trigger for pelvic torsion is a a specific type of iliacus dysfunction in which the iliacus on one side of the body and the psoas on the other side of the body both become locked short.
The result is that the pelvis is pulled into a twisted pattern commonly called pelvic torsion.
Pelvic torsion has two primary impacts on the body:
1) It causes a functional leg-length discrepancy that throws the body off its center line of balance...
2) This triggers a chain reaction of muscular compensation resulting in pain and strain that can’t be diagnosed by looking at isolated parts of the body only.
Muscles forced to compensate in this way are literally in a struggle against gravity.
This struggle means that pain or strain can be produced virtually anywhere in the body.
what to do
If you believe that iliacus dysfunction and pelvic torsion may be at the root of your symptoms, I strongly urge you to view the first 5 lessons excerpted from my course, “Postural Blueprint for Correcting Pelvic Torsion.” These are FREELY available and will help you determine if this condition applies to you.
Learn more about ONLINE COURSE WORK HERE
Stephen O’Dwyer, Neuromuscular Therapist and Pain Relief Researcher - has been helping individuals achieve significant and often permanent relief for chronic, stubborn and "unexplained" pain for over 30 years.
His learning platform, Relieving That Pain Online Courses, is dedicated to detailed instruction and actionable tools of self-care for individuals seeking help with pain for which the diagnosis has been vague or inconclusive.